Vagina 101: Anatomy, function, and what to look out for
Follows NC° Editorial Policy
At Natural Cycles, our mission is to empower you with the knowledge you need to take charge of your health. At Cycle Matters, we create fact-checked, expert-written content that tackles these topics in a compassionate and accessible way. Read more...
Key takeaways
- The vagina is an internal female reproductive organ that plays a vital role in sex, reproduction, birth, menstruation, and immunity
- There are many anatomical components to the vulva and vagina, including the clitoris, urethra, and vaginal walls, and each has its own function
- Your vagina is influenced by hormonal changes throughout your life and can be susceptible to several types of infections
- You can keep your vagina healthy by not washing it with soap, strengthening your pelvic floor muscles, and conducting regular self-checks and medical examinations
On this page
- What is the vagina?
- What does your vagina do?
- Vagina anatomy
- What are the most common vaginal problems?
- What are some common signs or symptoms of conditions involving my vagina?
- What are the common tests to check the health of your vagina?
- Tips to keep your vagina healthy
- When to see a doctor
- Take care of your vaginal health with Natural Cycles
The vagina is a small but mighty part of your reproductive system, and there is a lot to learn about it! Let’s look at the vagina anatomy, the roles each part plays in our bodies throughout our lives, and how to keep your vagina healthy.
What is the vagina?
The vagina is part of the internal female reproductive organ that connects the uterus with the outside of the vagina, the vulva, via the cervix [1]. Though the word “vagina” is often used to describe several parts of the reproductive system, the vagina is only one part of the overall reproductive anatomy. We will explain this in more detail later in the article.
What does your vagina do?
The vagina is an amazing organ, playing a vital role in reproduction, birth, and sex. Let’s take a closer look at some of the functions of the vagina:
- Sex: The walls of the vagina contain nerve endings (such as the G-spot) that provide some of the stimulation you may feel during intercourse [2]. Sexual arousal also helps the vagina release fluid that reduces friction during sex [3].
- Menstruation: When the uterus lining sheds during your period, it exits through the vagina [4]. Some people choose to insert tampons or menstrual cups into the vagina to collect blood, while others prefer to let it flow out of the vagina to collect in pads or period underwear.
- Pregnancy: When sperm are released inside the vagina (usually through penetrative sex), they swim through the cervix and deep into the reproductive system and fallopian tubes. If this happens during the fertile days of your menstrual cycle, the sperm cell might fertilize an egg cell, which can lead to pregnancy [5].
- Childbirth: If you give birth via a vaginal delivery, the baby travels from the uterus, through the vagina (sometimes called the birth canal), to get to the outside world. The vagina can stretch significantly during childbirth to allow the baby to pass through it [6].
- Immunity: The bacteria and acidic pH level of the vagina act as a barrier protecting germs from reaching the uterus [7].
Vagina anatomy
Every vagina has a similar anatomy, but the color, shape, size, discharge, and odor vary from person to person, and each individual's vagina can also change throughout their lifetime.
Where is your vagina located?
Your vagina is located inside your body, connecting the uterus and cervix to the outside world. The vaginal opening can be seen between your legs using a handheld mirror. You can locate it below the urethra (where you pee from) and above your anus.
Outside of the vagina: The vulva
The area we can see on the outside of the vagina is called the vulva. It forms the first line of defence against germs and consists of several different parts, including [8]:
- Labia: The folds of skin, or inner and outer lips, on either side of the vaginal opening are called the labia minora and labia majora, respectively [9].
- Clitoris: Located at the top of the labia and extending deep into the body, the parts of the clitoris we can see are the glans and clitoral hood [9]. This collection of nerves plays an important role in sexual pleasure [10], and during an orgasm, the muscles beneath the clitoris contract and tense [7].
- Vaginal opening: Connecting the vagina to the outside of your body, this is where a penis, sex toy, or fingers may be inserted during sex, a menstrual cup or tampon may be inserted during your period, where a baby is pushed through during birth, and where menstrual blood is released through.
- Urethra: This is the tube through which you urinate. It is in close proximity to the rectum and vagina, and is shorter in female bodies than in male ones, which is why women (and those with a female reproductive system) are more susceptible to urinary tract infections (UTIs) [11].
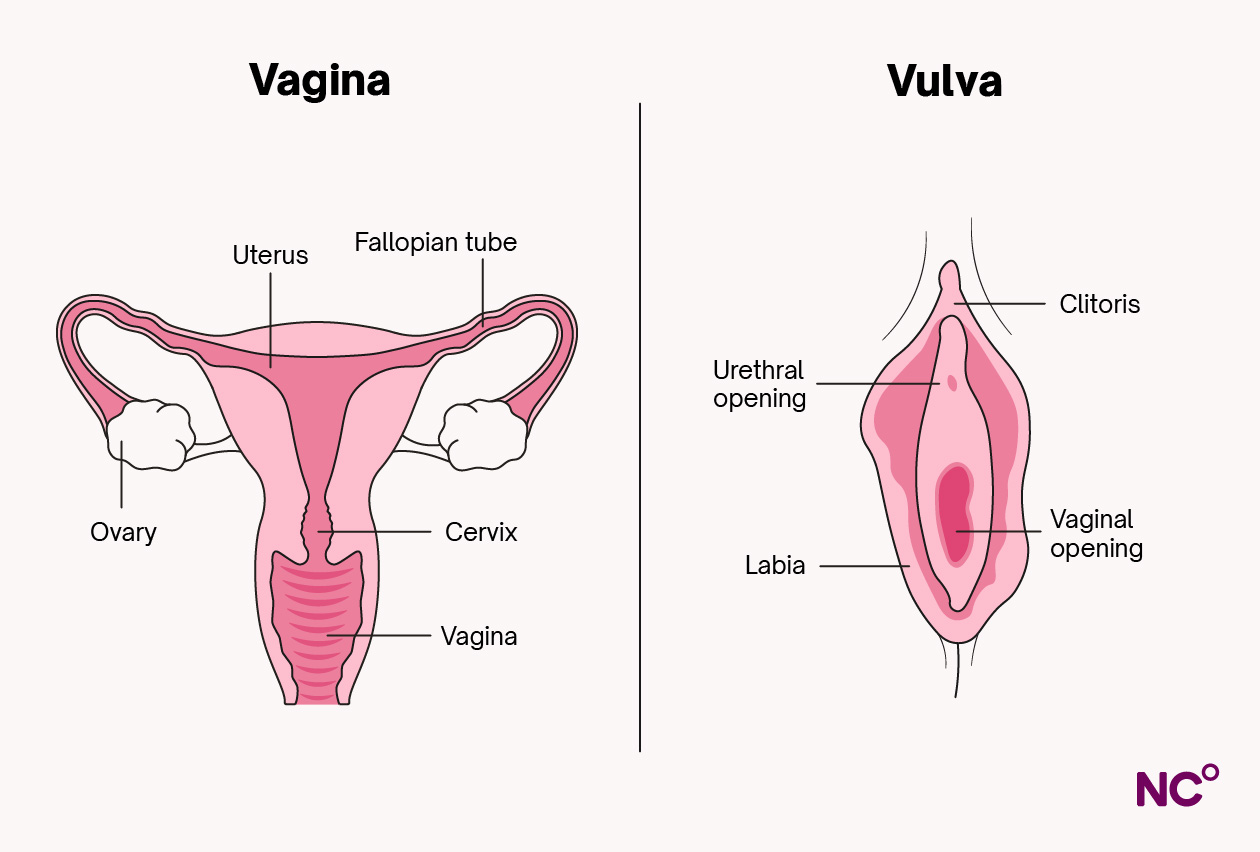
Inside the vagina
Your vagina is a funnel-shaped organ that connects the vaginal opening to the uterus via the cervix [1]. The average depth of a vagina can be anywhere between 7 and 10cm [3]. It is muscular and stretchy, with ridged walls that join to create a tube-like structure. These walls facilitate the secretion of vaginal fluids, contain nerve endings for sexual pleasure, and have receptors for estrogen [3]. Estrogen is crucial for maintaining a healthy vaginal lining and supporting the healthy bacteria that keep your vagina at a slightly acidic pH level [9].
How the vagina changes during the menstrual cycle
Your vagina changes throughout the phases of your menstrual cycle, especially in terms of its secretions. Vaginal discharge is present throughout your cycle, maintaining pH balance and lubrication. But the amount and type of discharge changes depending on which phase of your cycle you are in.
At the start of your cycle, you are on your period, and your menstrual blood flows from your uterus, via your cervix, and out through your vagina [4]. In the late follicular phase, as your period ends and you approach ovulation, you are more fertile, and estrogen levels rise. This hormonal change increases the amount of cervical mucus you produce, leading to clear, stretchy discharge resembling egg white [12, 13]. High estrogen levels also increase libido and stimulate your vaginal walls to produce more fluid, so you may find you have more lubrication during sex [3, 14].
After ovulation, the luteal phase begins. Estrogen levels drop, and progesterone levels rise. Cervical mucus reduces, but you may notice an increase in vaginal discharge [15]. Luteal phase discharge often feels thicker and may look white or slightly yellow [16, 17]. As estrogen levels reduce, your vagina can produce less lubrication, and you may feel drier [18].
How the vagina changes during sex
Sexual arousal plays an important part in preparing the vagina for sex. When you are sexually aroused, glands at the opening of the vagina (Bartholin’s glands) and urethra (Skene’s glands) release a fluid to moisten the vagina and increase lubrication for penetrative sex [7]. There is increased blood flow to the vaginal walls, making them swell, and, if you reach orgasm, your vaginal muscles contract [19].
Arousal can sometimes be a slow process, which is why patience, communication, and, often, foreplay are really important. There are also lots of reasons you may not feel like having sex. Consent is necessary for all types of sex, and vaginal lubrication does not equal consent.
How the vagina changes as we age
Our hormones fluctuate throughout our lives, and there are a few milestone moments when age affects our vaginas.
Puberty: The start of our reproductive years, when increased estrogen and progesterone cause several emotional and physical changes to the body, including the vagina. Puberty typically begins between the ages of 8 and 13 for girls, with most experiencing their first period by the age of 13, though this can occur earlier or later [20]. Hormones during puberty also cause the labia to widen and change colour, ranging from light pink to dark red or brown, and pubic hair begins to grow [9]. Once our periods begin, hormones eventually settle into the typical menstrual cycle pattern described above.
Pregnancy: If you become pregnant, both estrogen and progesterone levels rise as a natural part of pregnancy. This can lead to more blood flow to the vagina and vulva, causing minor swelling and a darkening of the skin in the area [9]. Elevated hormones can also cause an increased amount of vaginal discharge, a higher risk of vaginal infections, and a change in the balance of vaginal bacteria [9].
Postpartum: After birth, breastfeeding can lead to vaginal dryness. If you have had a vaginal birth, the skin of the vulva and vaginal opening will stretch to allow the baby to be born, and you may have minor tearing [9]. It is normal for the skin to take time to heal and return to normal after giving birth, though you should speak to your midwife or doctor if you have any concerns.
Menopause: The moment when our periods end, determined retrospectively after 12 months without a period [21]. The time before this is perimenopause, and the time after is postmenopause. One of the most notable changes in our vaginal health during perimenopause is irregular periods. Erratically fluctuating estrogen during this time can also cause vaginal dryness, itchiness in the vagina or on the vulva, and discomfort or pain during sex [22]. If you are affected by any of these symptoms, speak to your doctor, as treatments are available.
What are the most common vaginal problems?
Like any part of our body, there are some common vaginal problems many of us will encounter:
- Vaginitis: General soreness and swelling in the vagina or vulva is called vaginitis, and the causes of this condition can vary from infection to dryness to skin irritation [23].
- Yeast infections: The most common yeast infection is thrush, characterised by itching, soreness, and white, lumpy discharge [24]
- Bacterial vaginosis (BV): BV is a vaginal infection caused by an imbalance in vaginal bacteria, characterised by watery, grey, or fishy-smelling discharge [25].
- Sexually transmitted infections (STIs): STIs are passed from person to person via sexual contact (or, sometimes, needle usage or other physical contact), such as chlamydia, gonorrhea, or genital warts [26].
- Vaginismus: This is an involuntary reaction where the vaginal walls tighten, sometimes causing burning, stinging, and pain during sex. It usually happens when trying to put something inside the vagina, like a tampon, finger, sex toy, penis, or speculum during a medical appointment [27].
- Vaginal prolapse: Prolapse is when a pelvic organ (uterus, bladder, or rectum) descends towards the vagina. This can happen for a variety of reasons, including muscle weakness after childbirth or persistent constipation [28].
We know that some of these experiences can be distressing. If you have any concerns about your vagina or believe you have any of these conditions, speak to your doctor or sexual health clinic for tailored guidance.
What are some common signs or symptoms of conditions involving my vagina?
The symptoms you experience will depend on the condition you have. But common symptoms to look out for that may signal something unusual include:
- Discharge changes
- Itching or burning
- Pain during sex
- Bleeding during or after sex
- Dryness
- Odor changes
Often, these symptoms are very treatable, but in rare cases may indicate something serious. Speak to your healthcare provider if you are experiencing any abnormal symptoms.
Since vaginal discharge naturally changes throughout your cycle, one way to learn what is normal for you (and what is not) is to track your symptoms. The NC° app lets you log information about your discharge throughout your cycle, including colour, consistency, and amount, so you can see patterns and know when something is out of the ordinary.
What are the common tests to check the health of your vagina?
There are several tests you can take to check the health of your vagina and reproductive system. Some are regular checkups, and others can be taken in response to symptoms.
Cervical screening, previously known as a Pap smear, checks the health of your cervix and tests for high-risk variations of the human papillomavirus (HPV), which can sometimes lead to cervical cancer. When you attend a screening appointment, a nurse or healthcare professional will give you a pelvic exam, then take a sample from your cervix using a soft brush. In some countries, self-testing is also available [29, 30].
Screening is usually available for anyone with a cervix between the ages of 21 and 65, depending on where you are located, and is recommended every three to five years (if you are an NC° app user, we’ll give you a yearly reminder!).
We know that cervical screening tests can be daunting and uncomfortable, especially if you experience conditions like vaginismus, but it’s important that you don’t skip these appointments.
Your healthcare provider or sexual health clinic can provide tests for vaginal or sexually transmitted infections. If you believe you may have thrush or BV, a pH test can confirm whether your pH balance is unusual. There are also some at-home tests available for common infections, including thrush, BV, and chlamydia, but it is a good idea to speak to a medical professional in the first instance if you think you have an infection.
How to do a self-exam of your vagina
You are more likely to spot changes to your vulva and vagina if you do a regular self-examination of the area. All you need is a mirror and a bright room (or flashlight). Always wash your hands before and after the exam, and try to choose somewhere warm and quiet where you won’t be disturbed.
Step 1: Remove your clothes from the waist down, and lie with your legs spread apart and your knees bent. It can also help to prop yourself up against a wall with a pillow.
Step 2: Use a handheld mirror to look between your legs so you can see the vulva area. You may want to use a flashlight to see better.
Step 3: Identify the vaginal opening (above the anus and below the urethra). Gently use your fingers to part the labia so you can see inside your vagina better.
Step 4: The vagina should be a dark red color, and you may be able to see the ridges in the vaginal wall. Look out for any unusual discharge, lumps, spots, irritation, or changes in colour.
Step 5: If you feel comfortable, you can gently insert a finger inside the vagina and feel the vaginal walls. You might be able to feel the cervix, though it changes position throughout your cycle and isn't always easy to reach.
Try to do your self-examinations around the same time each month — as we know from earlier, the vagina changes throughout the cycle. You can even tie your check-in to a self-breast exam, if it helps you remember! Self-exams are a great way to get to know your body and keep on top of your vaginal health. But remember that at-home checks do not replace medical checks such as cervical screening.
Tips to keep your vagina healthy
Alongside self-exams and medical checks, there are lifestyle choices you can make to support a healthy vagina.
Don’t use soap in your vagina
Your vagina is self-cleaning, so there is no need for any additional cleaning inside your vagina. Doing so can lead to an upset in the microbiome and increase your risk of infection [8]. You can, however, gently clean your vulva using warm water. If you do wish to use soap to clean your vulva, choose a pH-balanced, unscented option. Always wash from front to back when cleaning this area, starting with your labia, then your perineum, then your anus.
Strengthen your pelvic floor
Pelvic floor muscles support the bladder and bowel, and in women, they also support the uterus and vagina [31]. Keeping your pelvic floor muscles strong aids bladder and bowel control, contributes to core stability, and can improve sexual function [31]. General aging and life events, like giving birth vaginally, can weaken pelvic floor muscles, but you can strengthen them through pelvic floor exercises, just like any other muscle.
Practice safe sex
Sex can introduce infection into your vagina, causing uncomfortable symptoms and, sometimes, if left untreated, sub- or infertility. But practicing safe sex can help protect you from unwanted infections. Only barrier methods, such as condoms, can protect you from STIs. Visit your sexual health clinic for an STI check if you notice any symptoms or if you are regularly having unprotected sex with new partners. Even if you are in a long-term relationship, it is a good idea for both partners to have a sexual health check before choosing to use non-barrier methods of birth control. If you have an infection or believe you have been exposed to an STI, seek medical advice and, in the meantime, abstain from sex until you have been treated, to stop further spread of the infection to others.
When to see a doctor
You should always speak to your healthcare provider if you are concerned about the health of your vagina, particularly if:
- You notice a change in the texture, colour, or smell of your discharge
- You notice any unusual lumps on the vulva or inside the vagina
- You experience irregular bleeding between periods
- You experience pain or bleeding during or after sex
- Your vulva or vagina is itchy or irritated
- You think you have had sex with someone who has an STI
- You are pregnant
Visiting your doctor to speak about your vaginal health may feel embarrassing or daunting, but healthcare professionals and OBGYNs look at vaginas every day and want to help. Remember that you can always request to see a female doctor or nurse for your appointment, or ask for a chaperone to be present at the appointment if you prefer to have someone else in the room with you and the clinician.
Take care of your vaginal health with Natural Cycles
Learning more about your body throughout your cycle is an empowering way to feel in control of your health. Natural Cycles uses biomarkers (such as temperature data) and its one-of-a-kind algorithm to help you track the phases of your menstrual cycle. You know when you are at your most fertile, and predict when your period is likely to arrive.
The NC° app makes it easy to record symptoms like PMS, pain, discharge, and spotting, so you can spot patterns throughout your cycle. Whether you are looking to plan or prevent pregnancy, or simply want to know more about your body, Natural Cycles is here to help.
Did you enjoy reading this article?
